23
Managing Opioid Constipation: A Guide to PAMORAs
PAMORA Selection Assistant
Disclaimer: This tool is for educational purposes only. Always consult with a licensed healthcare provider before starting or changing any medication. Warning: PAMORAs are strictly contraindicated if you have a mechanical bowel obstruction.
Select the medication you want to learn more about to see its specific profile and clinical considerations:
Methylnaltrexone
(Relistor)
Fastest OnsetNaloxegol
(Movantik)
Daily Oral UseNaldemedine
(Symproic)
Chronic OICFor anyone taking opioids for chronic pain or palliative care, the struggle with the bathroom is often more than just an annoyance-it can be a debilitating part of the treatment. Opioid-induced constipation, or OIC, isn't like your typical digestive slowdown. It is a specific medical condition where the medication itself shuts down the gut's natural movement. For many, standard over-the-counter laxatives simply don't cut it, and some patients find the side effects so severe they consider stopping their pain medication entirely.
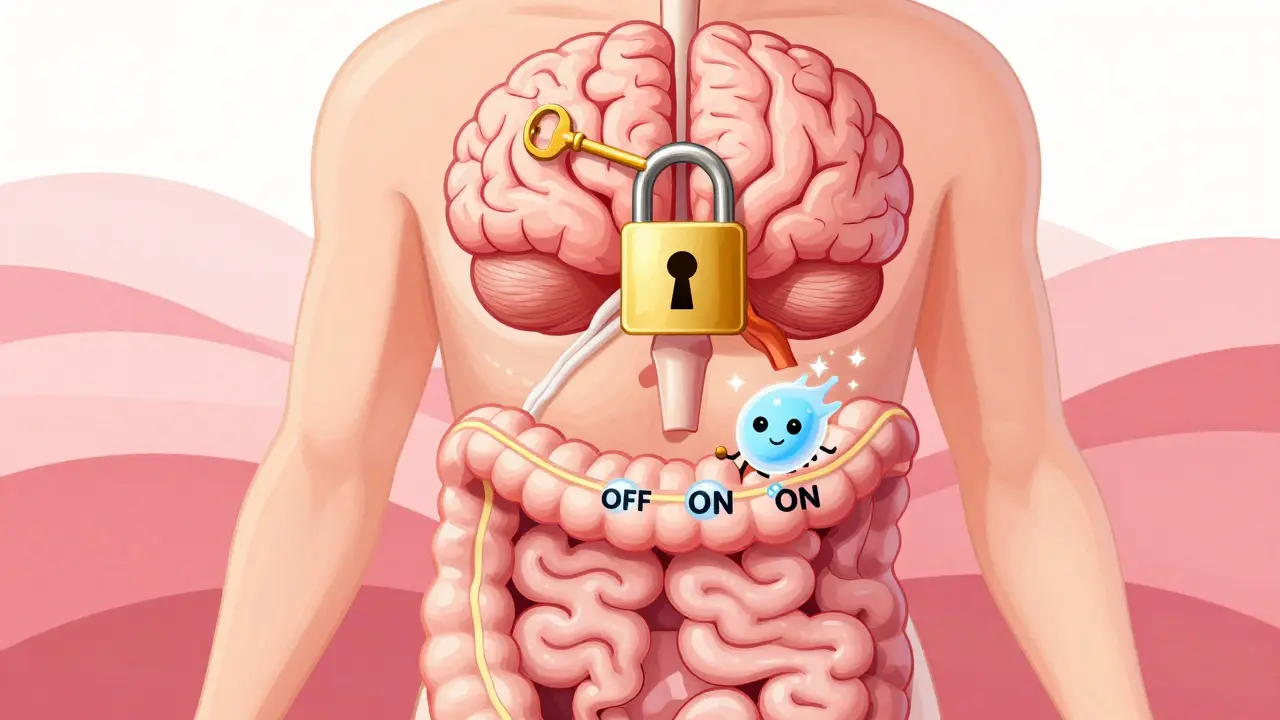
This is where Peripherally Acting Mu-Opioid Receptor Antagonists is a class of medications, known as PAMORAs, designed to block the constipating effects of opioids in the gut without stopping the pain-relieving effects in the brain. Essentially, they act like a "selective switch," turning off the opioid effect in your intestines while leaving the pain relief active in your central nervous system.
Why standard laxatives often fail
To understand why you need a PAMORA, you first have to understand what opioids do to your insides. Your gut is lined with a dense network of mu-opioid receptors . When these receptors are activated by pain medication, they stop the rhythmic contractions (peristalsis) that push waste through your system. They also interfere with how your gut secretes fluids and absorbs water, leaving stool hard and difficult to pass.
Traditional laxatives usually just add water to the stool or irritate the bowel lining to force a movement. They don't address the root cause. Research shows that fewer than 30% of chronic opioid users maintain regular bowel function using only these traditional methods. PAMORAs are different because they target the actual receptor causing the blockage, treating the cause rather than just the symptom.
Breaking down the PAMORA options
Not all PAMORAs are the same. Depending on your medical history, whether you are treating cancer-related pain, and your kidney function, your doctor will choose a specific agent. The three most common are Methylnaltrexone, Naloxegol, and Naldemedine.
Methylnaltrexone (brand name Relistor) is often the first choice for those needing a quick response. Because it has a charged molecular structure, it cannot cross the blood-brain barrier, meaning it won't interfere with your pain relief. It's available as a subcutaneous injection-which is helpful for patients in palliative care-and as an oral tablet. In clinical trials, over 50% of patients had a bowel movement within just four hours of administration.
Naloxegol (brand name Movantik) is a pegylated derivative of naloxone. This "pegylation" process essentially keeps the drug in the peripheral areas of the body and out of the brain. It is taken orally once a day and is generally preferred for patients with non-cancer pain who want a simple daily pill.
Naldemedine (brand name Symproic) also uses a polyethylene glycol chain to ensure it stays out of the central nervous system. It has shown a strong response rate in trials, with nearly 48% of patients achieving spontaneous bowel movements during the COMPOSE-3 study.
| Feature | Methylnaltrexone | Naloxegol | Naldemedine |
|---|---|---|---|
| Delivery Method | Injection & Oral | Oral only | Oral only |
| Onset Speed | Very Fast (Hours) | Moderate (Days) | Moderate (Days) |
| Primary Use Case | Cancer & Non-cancer | Chronic Non-cancer | Chronic OIC |
| Renal Caution | Dose reduction needed | Contraindicated (Severe) | Standard Monitoring |
Real-world performance and trade-offs
While these drugs are a lifesaver for many, they aren't without their hurdles. The most common complaint from patients is the cost. Without insurance or manufacturer coupons, these medications can cost thousands of dollars per year, making them inaccessible for a large portion of the population. Some patients also report severe abdominal cramping as the gut "wakes up" after being dormant.
There is also a theoretical risk that blocking peripheral receptors could slightly reduce the overall pain-killing effect of your opioids, since some analgesia actually happens in the gut. However, most clinical evidence suggests that at therapeutic doses, you won't feel a return of your pain. The bigger concern is for those with a mechanical bowel obstruction-if your gut is physically blocked, using a PAMORA can be dangerous and is strictly contraindicated.
Practical tips for starting treatment
If you're starting a PAMORA, don't expect a "magic pill" that works instantly for everyone. There is often a 2-3 week learning curve to find the right dose. Many patients are initially underdosed, which leads them to think the drug isn't working when they actually just need a titration adjustment.
Timing is also key. For the best results, try to time your PAMORA dose about one hour before the peak effect of your opioid medication. This helps keep the gut moving throughout the day. Additionally, keep a simple log of your bowel movements and any cramping; this data is invaluable for your doctor when deciding if a dose increase is necessary.
Looking ahead: The future of OIC management
The market for opioid-induced constipation treatment is evolving. We are seeing the development of dual-action drugs that combine a PAMORA with a 5-HT4 agonist, which essentially pushes the gut from two different directions. There are also biosimilars entering the pipeline, which should eventually bring the cost down and make these therapies available to more than just the privileged few.
Will PAMORAs make my pain medication stop working?
No, that is the primary advantage of PAMORAs. Unlike traditional opioid antagonists (like naloxone used for overdoses), PAMORAs are designed to be "peripherally acting." This means they cannot cross the blood-brain barrier in significant amounts, so they block the receptors in your gut but leave the receptors in your brain alone, preserving your pain relief.
Can I take PAMORAs if I have a bowel obstruction?
Absolutely not. All PAMORAs are contraindicated in patients with a known or suspected mechanical gastrointestinal obstruction. Forcing the bowel to contract when there is a physical blockage can lead to serious complications.
What is the difference between OIC and regular constipation?
Regular constipation is often caused by diet, dehydration, or lifestyle. Opioid-induced constipation (OIC) is iatrogenic, meaning it is caused by a medical treatment. Opioids bind to mu-receptors in the enteric nervous system, which actively suppresses motility and fluid secretion, making it much harder to treat with standard fiber or mild laxatives.
Are there side effects I should watch for?
The most common side effects include abdominal pain, nausea, and cramping. Because these drugs stimulate the gut, some people experience a sudden "rush" of bowel activity which can be uncomfortable initially. If you experience severe dizziness or an allergic reaction, contact your provider immediately.
How long does it take for these medications to work?
It depends on the drug. Methylnaltrexone can work very quickly, often within 4 hours. Others, like Naloxegol, may take a few days of consistent daily use before you notice a significant and steady improvement in your bowel habits.