Epigastric pain: what it usually means and what to do now
That dull or sharp ache right under your ribs in the center of your upper belly? That’s epigastric pain. It can be a minor annoyance from what you ate or a sign of something that needs prompt care. This page gives quick, practical steps you can try at home, explains common causes, and tells you when it’s time to call a doctor or go to the ER.
Common causes — quick check
Start by thinking about timing and triggers. Pain right after eating, spicy food, or alcohol often points to heartburn, acid reflux, or gastritis. A burning ache that improves with antacids suggests acid-related issues. Pain that comes with fever, severe nausea, or constant vomiting could be infection or inflammation like pancreatitis or a peptic ulcer. Sharp, sudden pain that spreads to your back or shoulder can mean something more serious — gallbladder, pancreas, or even a cardiac issue in rare cases.
Medications matter. NSAIDs (like ibuprofen) and some antibiotics can irritate the stomach lining. If you’re on drugs such as blood pressure meds or heart meds, they can change how your stomach feels. If you’ve used over-the-counter remedies and nothing helps, note any recent changes in medication or new supplements.
Simple things you can try right away
1) Adjust what you eat — avoid fatty, spicy, or acidic foods for 24–48 hours. Eat smaller meals and don’t lie down right after eating. 2) Try an over-the-counter antacid or an H2 blocker (famotidine) for short-term relief. 3) Sip clear fluids and avoid alcohol, caffeine, and smoking. 4) Use heat — a warm pack on the upper belly can ease muscle tension. 5) If you take NSAIDs regularly, stop them for a day or two and see if pain improves; ask your doctor about safer options.
These measures help many people, but they’re not a fix for everything. If you use antacids often, or symptoms return repeatedly, you should get checked for underlying problems like ulcers or GERD.
Worried about related conditions? We have practical reads on treatments and drug options that connect to upper belly issues — for example, alternative meds for stomach problems and safety tips for antibiotics and anti-nausea drugs. Check our pieces on Motilium and Cytotec alternatives if your symptoms relate to digestion or gastric motility.
When to get urgent help: severe, sudden pain; vomiting blood or black stools; fainting or low blood pressure; trouble breathing; high fever with worsening pain. Also see a doctor if pain lasts more than 48–72 hours, wakes you at night, or keeps you from eating and drinking.
Keep a short note of when the pain started, what you ate, any new medicines, and any other symptoms. That makes your visit faster and more useful. If you’re unsure, calling your primary care or a nurse line for advice is a good first step. Epigastric pain is common — but a smart, quick response helps you avoid complications and get the right care fast.
30
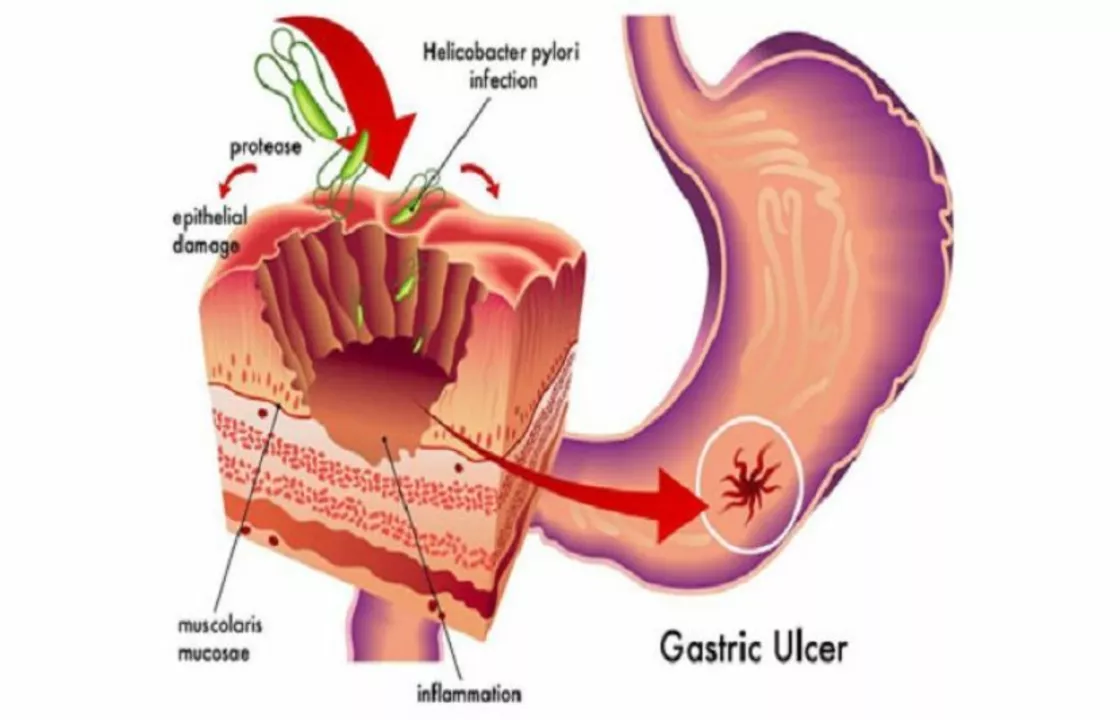
The Connection between Epigastric Pain and H. Pylori Infection
In my latest blog post, I explored the connection between epigastric pain and H. Pylori infection. Epigastric pain, which is the discomfort felt in the upper abdomen, can sometimes be linked to H. Pylori, a type of bacteria that can cause stomach ulcers. I discovered that this bacteria can also lead to gastritis, which may further contribute to the sensation of pain in the epigastric region. It's important to get tested for H. Pylori if you're experiencing persistent epigastric pain, as early detection and treatment can help prevent complications. Stay tuned for my next post, where I'll discuss treatment options and ways to prevent H. Pylori infection.
Latest Posts
Popular Posts
-
 Five Essential Rules for Taking Medication Safely
Five Essential Rules for Taking Medication Safely
-
 How to Manage Multiple Pharmacies and Prescribers Safely
How to Manage Multiple Pharmacies and Prescribers Safely
-
 Questions to Ask About Your Prescription Label at the Pharmacy
Questions to Ask About Your Prescription Label at the Pharmacy
-
 Future of Digital Pharmacy: Predictions for Generic Medication Delivery
Future of Digital Pharmacy: Predictions for Generic Medication Delivery
-
 Mandatory vs Permissive Substitution: Key State Law Differences in Pharmacy Practice
Mandatory vs Permissive Substitution: Key State Law Differences in Pharmacy Practice