Skin Rashes: Quick Help, Causes, and When to See a Doctor
A rash can show up overnight and freak you out. Most rashes are harmless and treatable at home, but some need urgent care. Below you’ll find easy ways to identify common rashes, simple first-aid steps you can try right now, and clear signs that mean you should see a doctor.
Common Causes & How to ID Them
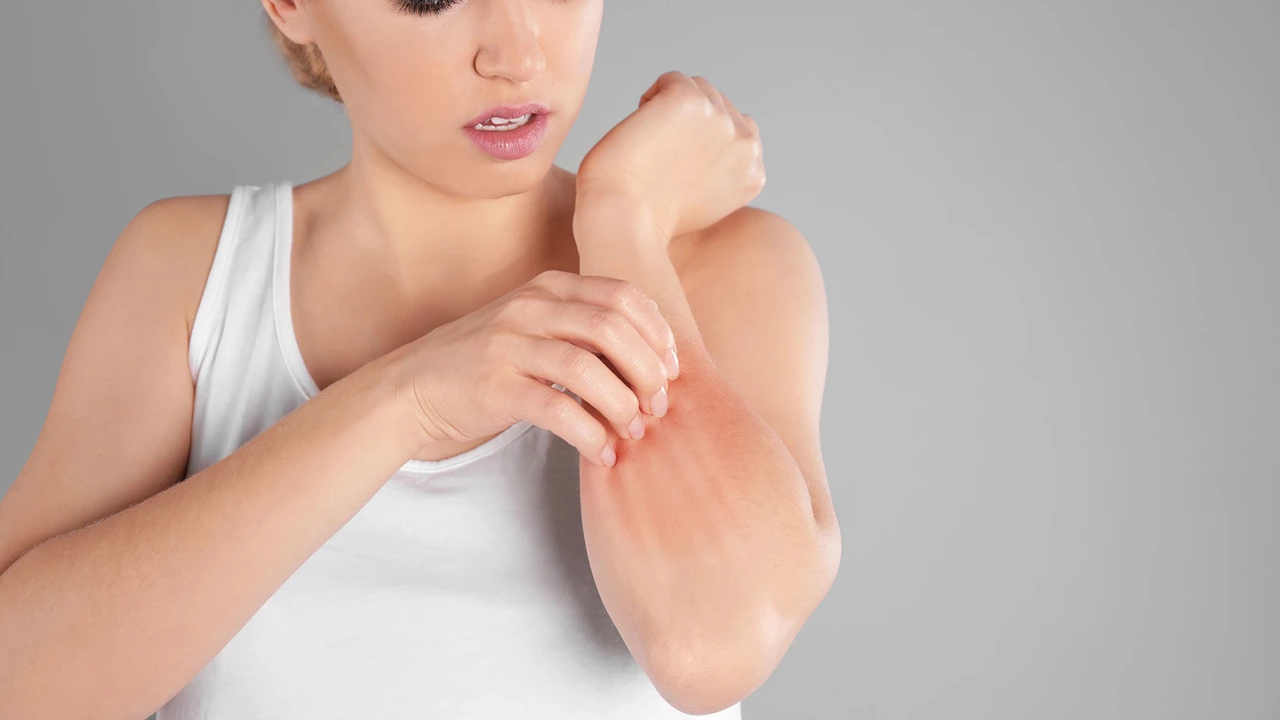
Contact dermatitis looks like redness and itching where skin touched something — think new soap, nickel jewelry, or poison ivy. If it’s limited to where the item touched your skin and gets better when you stop contact, that’s a give-away.
Eczema (atopic dermatitis) is dry, scaly, and often in creases of elbows and knees. It’s chronic and flares with stress, heat, or irritants. Psoriasis usually makes thicker, well-defined scaly patches, often on elbows, knees, or scalp.
Fungal rashes (ringworm, athlete’s foot) are often round with clearer center and a red, spreading edge. Shingles starts as painful blisters on one side of the body along a nerve path. Bacterial infections show redness, warmth, swelling, and sometimes pus.
Drug rashes can appear a few days to weeks after starting a new medication. Common culprits include some antibiotics, NSAIDs, and certain blood pressure drugs. If a rash appears after a new medicine, tell your doctor right away.
First Aid and When to Get Help
For mild rashes: cool compresses, gentle soap, and fragrance-free moisturizers help. Over-the-counter 1% hydrocortisone cream calms inflammation for short-term use. Oral antihistamines (cetirizine or loratadine) reduce itching at night.
Avoid scratching — keep nails short, wear cotton clothing, and use a cold pack for intense itching. For suspected fungal rashes, an antifungal cream works well; if it doesn’t improve in 2 weeks, see a provider.
Go to a doctor now if the rash spreads quickly, covers a large area, or comes with fever. Seek immediate emergency care for swelling of the face or throat, trouble breathing, dizziness, or very painful, blistering rashes. These can be signs of severe allergic reaction or serious infection.
Bring helpful info to your appointment: photos of the rash from different days, a list of new products or medicines, and any recent travel or insect bites. A short course of a stronger prescription cream, oral antibiotics, or an allergy workup might be all you need.
Finally, protect healing skin: avoid strong detergents, sunburn, and hot showers. Small changes — switch to mild cleaners, keep skin hydrated, and avoid known triggers — often stop rashes before they get worse. If you’re unsure, calling a nurse line or making a quick appointment can save time and headaches.
18
The Connection Between Skin Rashes and Gastrointestinal Issues
As a blogger, I've always been intrigued by the connection between our skin and our overall health. Lately, I've been researching the link between skin rashes and gastrointestinal issues. It turns out that skin flare-ups may be a sign of an underlying gut problem, such as an imbalance of gut bacteria or food sensitivities. Inflammation in the gut can cause inflammation in the skin, which then presents itself as eczema, psoriasis, or other rashes. So, if you're experiencing persistent skin issues, it might be worth looking into your gut health and making necessary adjustments to your diet and lifestyle.